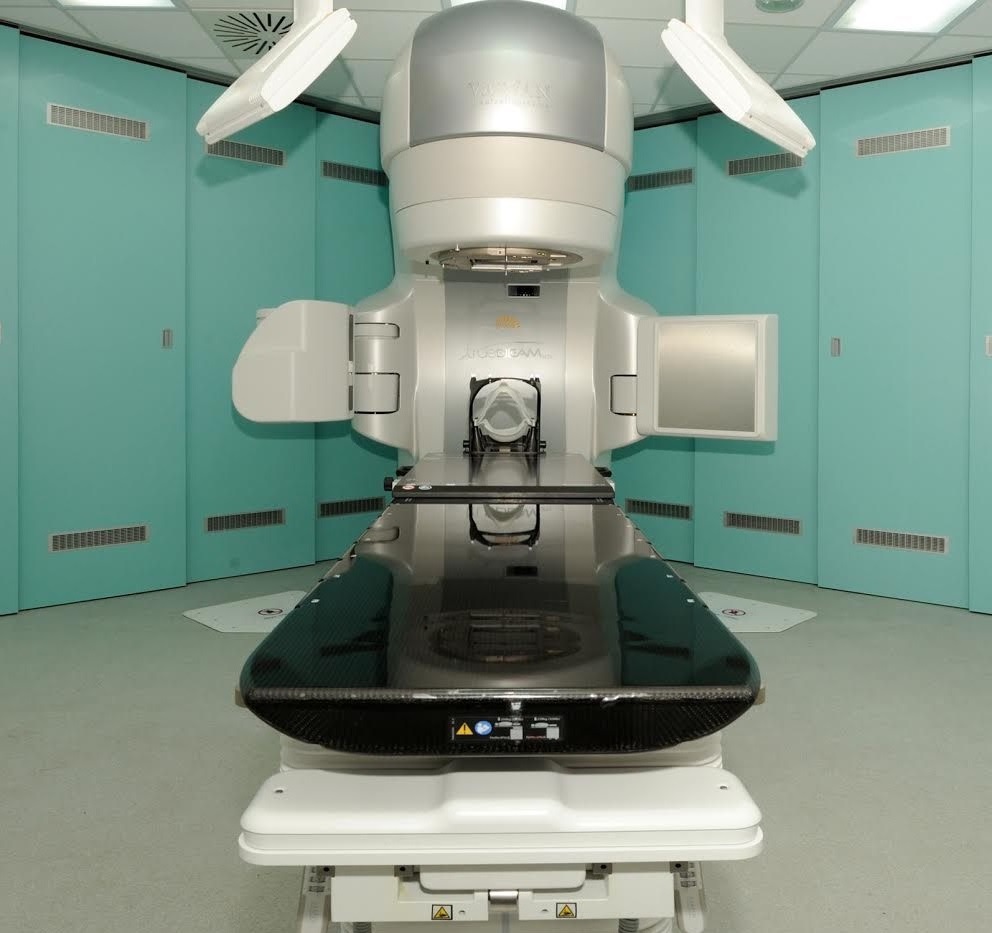
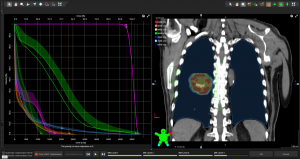
The Radiotherapy Physics section is responsible for providing scientific services to the Radiotherapy Department of St Luke’s Cancer Centre, which serves a population of 1.4 million in Surrey and West Sussex and with a satellite facility at East Surrey Hospital. The Centre offers a range of advanced radiotherapy techniques including:
- Intensity modulated radiotherapy (IMRT); >90% of radical radiotherapy treatments are delivered using this advanced technique
- Stereotactic Ablative Radiotherapy (SABR) for primary lung cancer and oligometastases. The department has been commissioned by NHS England to deliver this service, and was one of three UK centres appointed to provide a mentoring service to help develop SABR nationally.

- Motion management, including breath-hold techniques to reduce normal tissue toxicity.
- A comprehensive brachytherapy service including image-guided brachytherapy (IGBT) treatments and an internationally renowned prostate seed service.
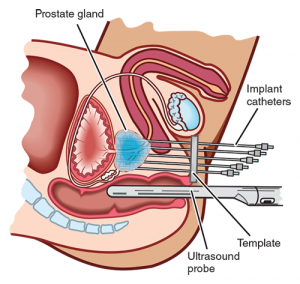

- A contact radiotherapy service for rectal cancer
- In 2020, the department will be installing a Varian ETHOS Therapy unit, giving the capability for online adaptation of the radiotherapy treatment

Excellent links exist with the National Physical Laboratory and a joint consultant physicist post has been appointed to help develop NPL’s clinical services. This has led to national dosimetry intercomparisons involving all UK radiotherapy centres for stereotactic radiosurgery (SRS), SABR, VMAT and High Dose Rate brachytherapy demonstrating consistent radiation dose delivery to patients across the UK for these complex treatments. This work has been in collaboration with the National Cancer Research Institute’s (NCRI) Radiotherapy Trials QA group and has also acted as a means of accreditation for clinical trials, thus increasing patient uptake with these advanced radiotherapy techniques.
The section also has links with equipment manufacturers. Through collaboration with Varian Medical Systems, the department performed beta-testing of the knowledge-based radiotherapy treatment planning system, RapidPlan, and delivered the first treatment worldwide planned with this software. As part of an ongoing collaboration with Mirada Medical Ltd, the department are testing auto-contouring software designed to streamline the delineation of tumours and normal tissues.
The Section is also responsible for ensuring the Trust meets the statutory obligations of the Ionising Radiation Regulations 2017 and the Ionising Radiation (Medical Exposure) Regulations 2017 with regard to radiotherapy, national dosimetry codes of practice and national guidelines. In order to meet this statutory requirement, the team has to work to a high level of expertise and implement national and international standards of dosimetry and safety. The Whole Time Equivalent establishment is currently approximately 25 physicists and 10 dosimetrists / treatment planners. The section is divided into three services:
Each section is actively involved in research and development in a range of different areas.
Of course its not all hard work and the team regular have social meetups!